Are hospitals in the US running out of covid-19 treatments?
Covid-19 hospitalizations are inching closer to their historic records seen one year ago. Some begin to ration treatments as they feel the pressure.
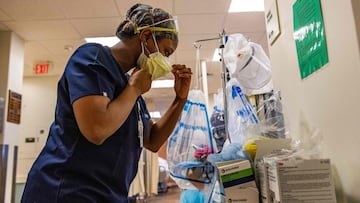

Hospitals around the country are feeling the pressure of Omicron as treatments become scarce and staffing hits critical levels.
The Centers for Disease Control and Prevention reported that currently almost 15,000 covid-19 patients are being hospitalized each day, an increase of more than 63 percent over the rate captured last week.
While Dr. Anthony Fauci has shared data from various countries and studies showing that Omicron typically leads to less severe infection, he has reiterated that though the risk of hospitalizations is lower, when coupled with a massive surge in cases, hospital systems could still be strained. Public health officials have been optimistic that the hospital system will be able to withstand the Omicron wave, but the New York Times is reporting that many hospitals are running out of treatments like monoclonal antibodies, and beginning to ration to patients with the highest need.
Treatment shortages
In 2021, the Food and Drug Administration approved the use of two covid-19 treatments shown to reduce the severity of covid-19 cases, which could keep hospitalizations at a manageable level. However, the chemistry needed to create these drugs is complicated and time-consuming. The first batch of Paxlovid, the drug produced by Pfizer was sent to states just before Christmas, and already some states have nearly depleted their supply. Places like New York City, are completely out of the drug, as it confronts the greatest surge in cases since 2020. In other states where supplies of the drug were sent to retail pharmacies like Rite Aid, some patients prescribed the drug have seen a price tag as high as $500 attached, discouraging many from filling their order.
The federal government has not been clear about when the next shipments will be sent. In a press conference this week, President Biden told the nation that he doubled the country's order to Pfizer and that within the next few months more than twenty million doses will arrive; the question is will they arrive fast enough to save patients during the brutal wave of infections facing the country.
Throughout the pandemic doctors around the world have shared various vitamin and drug cocktails, proven to help patients. With treatments running short, many hospitals are turning to these solutions.
Medical professionals sound the alarm
The Head of the White House Covid Response Team, Jeffery Zients on 5 January, said "We have the tools we need to manage this surge in Omicron cases." Zients spoke to the military medical professionals who have been sent to local hospitals and to efforts made by the government to "restock the medicine cabinet." While the measures taken are much needed, doctors and nurses on the ground are sounding the alarm that they do not have what they need to care for the patients in their care.
Michigan's chief medical executive, Dr. Natasha Bagdasarian expressed her concern over the shortages to the New York Times saying “There is simply not enough to meet the needs of everyone who is going to have Covid in the upcoming weeks and be at risk of severe complications." Adding that she does not believe "there is a way to make sure it gets to all the right people right now.” Hospitalizations in Michigan peaked in December 2021, decreased, and are up again. While the decrease helped, many supplies were exhausted, leaving staff with fewer options as Omicton takes hold in the state.
Staffing Shortages
Doctors, nurses, and other medical professionals are burned out, fatigued, and during this latest wave sick with covid-19. This comes as an average of one in five hospitals across the United States report experiencing critical staff shortages that are only expected to increase in the coming weeks. More than half of hospitals in Vermont and New Mexico have hit critical levels. Twenty-five states and territories are reporting critical personal shortages, an alarming fact when considering that hospitalizations are expected to continue to increase over the next few weeks.
Bed shortages
In twenty states, more than eighty percent of hospital beds are occupied.
Which states have surpassed eighty percent of their hospital bed capacity?
- AZ
- CT
- FL
- GA
- IN
- MA
- MD
- MI
- MN
- MO
- ND
- NH
- NV
- NY
- OH
- PA
- RI
- SC
- WA
- WV
Related stories
In Georgia which has seen hospitalizations nearly double in the last week is nearly hospital capacity with eighty-seven percent of ER beds and eighty-three percent of ICU beds are occupied. Concerning some officials in the state is how quickly pediatric hospitalizations have increased. On 21 December, twenty-two children were hospitalized within the Children's Healthcare of Atlanta system, and on 5 January that number was 118. Nearly three-quarters of these children have some sort of co-morbidity that makes them more vulnerable to the virus.
In Pennsylvania, Massachusetts, and Minnesota eighty-six percent of beds are in use, and trailing right behind are Washington, Rhode Island, and West Virginia.
